Healthy ageing is vital to social and economic development
Dr Margaret Chan, former Director-General of the World Health Organization (WHO), detailed how healthy ageing is vital to social and economic development in this article for our 2016 publication 'Facing the facts'.
 In almost every country, the proportion of older people in the population is increasing. By 2050, around 2 billion people in the world will be aged 60 years or over, with 400 million of them aged 80 years or over. Some 80 per cent will be living in what are now low or middle-income countries.
In almost every country, the proportion of older people in the population is increasing. By 2050, around 2 billion people in the world will be aged 60 years or over, with 400 million of them aged 80 years or over. Some 80 per cent will be living in what are now low or middle-income countries.
These demographic changes are closely entwined with socioeconomic development. Indeed, socioeconomic development can be considered as one of the causes of population ageing since it allows more people to survive childhood and childbirth, and has often been followed by dramatic falls in fertility.
These older populations are likely to present challenges to society through increased demand for health care, long-term care, social care and pensions. A greater proportion of older people also means a smaller proportion of those within the traditional range of working ages. These pressures have the potential to act as a brake on socioeconomic development, and much political discourse has focused on how the increased costs arising from them might be contained. Yet population ageing also presents significant opportunities.
As individuals, each of us benefits from being able to live longer, particularly if we can retain our health and the ability to do the things that are important to us. Older people make important social contributions as family members, volunteers and active participants in the workforce. Older populations thus represent a substantial human and social resource, albeit one that is currently under-utilised and poorly measured.
Health in older age will be a crucial determinant of where the balance lies between the costs and benefits associated with population ageing.
Good health enables older people to achieve the things they value, fosters their ongoing social participation (helping to prevent isolation), and has broader benefits for society by enabling their multiple contributions. Poor health undermines this engagement. It can also take a heavy toll on families who may need to provide care for a previously active family member or may become impoverished by health care costs.
These burdens are spread inequitably: those with the least resources, or who live in the poorest areas, are most at risk.
Investing in health at all ages
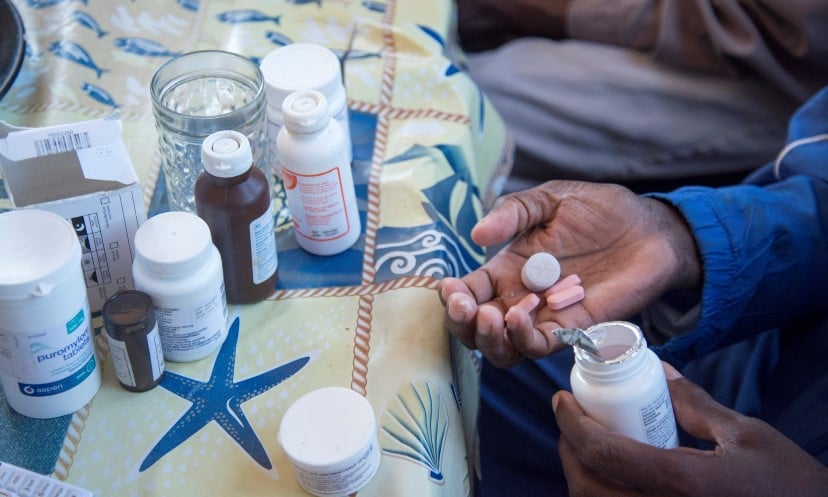
Building the systems that can foster good health across the life course therefore needs to be a central part of any policy response to population ageing.
Yet the debate on how to deliver better health has been narrow in scope, with persistent and outdated stereotyping of older people and a disjointed response to their needs. There are many misconceptions that need to be overcome. As a first step, we need to view the creation of these systems as an investment, rather than simply a cost. This investment has a solid economic return, not just in reduced costs or because it enables the myriad contributions of older people, but because it also releases capacity in the families that surround them.
So where should we make our investment if we are to foster good health in older age?
One focus of activity needs to be on preventing non-communicable diseases. Even in the poorest countries, the greatest health burdens for older people are from conditions such as heart disease, stroke, visual impairment, hearing loss and dementia. The impact of many of these conditions is two to three times greater for older people in low and middle-income countries than for those in high-income countries. Older people are also more likely to experience these disorders as multiple and coexisting problems. Loss of function through broader geriatric syndromes of frailty and impaired cognition, continence, gait, and balance are far better predictors of survival than the presence or number of specific diseases. Coordinated approaches to manage these co-morbidities and syndromes of older age are therefore a crucial part of our investment in health.
Refocusing health systems
Current health systems, particularly in low and middle-income countries, are often poorly designed to meet the chronic care needs that arise from this complex burden of disease. In many places, health systems need to move from focusing on the delivery of curative interventions for single acute problems to a more comprehensive continuum of care that links all stages of life and deals with multiple morbidities in an integrated manner. Yet, health systems often remain insufficiently sensitive to the specific needs of older people and fail to address even simple components of the care continuum.
Furthermore, good health for an older person is about more than the provision of health care. The physical and social environment – affordable transport, accessible streets and buildings, supportive communities and opportunities to participate – are also crucial for their well-being.
Building the cohesive, sustainable and just societies that can enable the participation of older people needs to be a core part of the post-2015 agenda.
Finally, we must not forget that towards the end of life, many people may require support to undertake even basic activities. But there are few standards or guidelines on appropriate ‘long-term care’. Family carers often lack an understanding of the challenges they face and care is often disconnected from health services. This can leave the needs of the older person inadequately addressed, with carers facing a greater burden than is necessary and acute care services being inappropriately used to fill chronic care gaps. Changing social patterns will make existing systems even less sustainable. The relative number of older family members is increasing dramatically; older people are less likely to live with younger generations and are more likely to want to continue living in their own home; and women, the traditional family carers, may have changing career expectations. Sustainable new systems of long-term care are therefore urgently needed. These should be focused on the individual rather than on the service; coordinated with health systems and designed to maintain the best possible function, well-being and social participation.
Investing in the systems that can provide this continuum of care across the life course, from the very young to the very old, may seem costly. But the cost of inaction is likely to be greater.
![]()
![]()
 Dr Margaret Chan is the former Director-General of the World Health Organization (WHO), appointed by the World Health Assembly on 9 November 2006.
Dr Margaret Chan is the former Director-General of the World Health Organization (WHO), appointed by the World Health Assembly on 9 November 2006.
Prior to joining WHO, she was Director of Health in Hong Kong. During her nine-year tenure as director, Dr Chan confronted the first human outbreak of H5N1 avian influenza in 1997. She successfully defeated the spate of severe acute respiratory syndrome (SARS) in Hong Kong in 2003. She also launched new services to prevent disease and promote better health.
 Follow us on LinkedIn
Follow us on LinkedIn
Stay up to date with the latest news, publications and features